*Content warning: This blog discusses and contains images of insulin pump, continuous glucose monitor (CGM), and blood sugar values, which can potentially be upsetting in relation to personal diabetes challenges. Please be advised of this before reading further.
I recently made the leap of faith to Tandem’s t:slim insulin pump with Control IQ software, and my mind is totally blown by all this tiny machine does akin to a normally-functioning pancreas each hour. Many others have chronicled their positive Tandem experiences, and at a later time I hope to join them with further blog posts. But the more pressing theme begging me to be written is one of design. Taking Stanford Medicine X training to heart, I’ve employed a discerning eye in the pros and cons of this pump from a user experience and design perspective.
Assumedly, the brilliant computer and biomechanical engineers at Tandem had their reasons for how they manufactured and coded this insulin pump. I’m not here to argue against their science, as this pump has already been life-changing in my own n=1 study within a few short weeks. I do not know if they consulted with any focus groups of people with diabetes in their creative processes, and I cannot falsely purport to represent everyone else’s opinions here. So with those disclaimers, for what it’s worth, here are my implementation and design 2 cents:
The Big Picture Design Pros:
If People magazine ranked the sexiest medical products on earth, this pump would be up there, just saying.
Having Dexcom tied right into the pump is not only helpful from an algorithmic, insulin-dosing standpoint. Simplified, it is one less clunky thing to carry. I still sometimes reach for my old Dexcom receiver out of habit, only to realize that now one small device clipped to my belt or slipped into my jeans pocket is simultaneously running the insulin show and serving as my Dexcom screen. (See also the diabetes online community (DOC) for enhanced pump clip suggestions!).
The algorithms…
provide far more input than any human being can possibly do each day. I plan to blog about the emotional aspects of this pump in the future, but to briefly convey it here- this concept has given me a level of peace after three decades’ worth of managing my own diabetes. People with diabetes are handed blunt instruments and routinely yelled at by society and medicine to essentially, “Just dose insulin and achieve ‘perfect’ control (which doesn’t exist, by the way), and no matter what happens, it’s all your fault!”. Watching this pump adjust my basal rate 32 times and microbolus twice, just in an overnight timeframe, to keep my blood glucose at a stable, safe line really hammered home how innovative this technology is, how much I wish everyone worldwide had easy, affordable access, and most glaringly, that what we have asked people to do for decades was never remotely possible. We tried our best, but we just plain can’t kickstart a faulty pancreas 32 times overnight, every night, forever.
Infusion sets
While I wish there had been more opportunities to test drive infusion set samples prior to the official pump start, I finally rationalized that kinked cannulas were one additional worry I did not need when returning to pumping after a long hiatus. Tandem’s TruSteel sets have been a breath of fresh air in terms of trusting that insulin is being delivered fully and properly, and the pain of having a needle set under the skin for a few days is negligible thus far when compared to the searing pain of needle-into-muscle from the past / competitor sets.


Built-in safety checks and balances
I feel comfortable that this pump will not accidentally bolus insulin in my sleep or if jostled in a crowd due to the many safety mechanisms included. The prompts explaining the basic steps involved with a cartridge and site change are helpful, too, as extra reminders of when to detach from the pump and what should happen next.
What I Would Change:
Again, see the disclaimers above. I am not saying Tandem did not have reasons for their current designs. But from a user point of view, I hope they will consider consulting with patient advocates and trying new ideas in future models.
Place the most important data in larger text on the screen!
My eyes are still functioning fairly well for my age, yet I am often frustrated by the pump’s tiny displays of numbers, which really matter in the diabetes experience. In my opinion, the Big Three are current Dexcom reading, insulin on board (IOB), and the amount of insulin being dosed via a bolus when applicable. To add a fourth option, current basal rate number would be helpful to have displayed upfront on the home screen, too.
Particularly when a bolus is occurring, the text at the bottom of the screen is far too small. I’d recommend Tandem take away approximately 1/3 of the Dexcom graph space on the home screen (the pink sticky note space in the example photo below), and use this bonus area to incorporate larger font for the data more frequently relevant to people with diabetes. For example, while it’s cool to see my blood sugar graph from the past 3 hours, I’d rather swap in some extra clicks to get to that particular graph than constantly have to jump to other screens to see my current basal rate or time of last bolus. Sacrifice that Dexcom graph space to personalize what the user wants to access easily in future models.


I’d additionally recommend inserting a “Favorites” option at the bottom of the home screen, similar to saving tabs in a web browser, in which the user can input screens they turn to often. For example, my personal preference is to go back in the History display and analyze boluses from the past few hours, which may inform how heavy a bolus I take now. Other users may find helpful meaning in Dexcom chart data from the past 12 hours, and wish to access that tab faster. If users could implement their own Frequently Utilized sort of list for themselves, this simplifies the diabetes management process even more so than this pump already does. At the end of the day, when people with diabetes are still piloting this plane, all of the little clicks and taps we make add up over time. How might we respect further design autonomy in future models?
Training / Communication
I can only speak for myself, and I want to be clear that this is not a gripe against the knowledgeable, compassionate Tandem representatives I spoke to many times over the phone, nor to my individual Tandem specialist trainer who calmly assisted in making this process doable and has been kind in yielding questions and checking in as needed. They are working within a larger, broken healthcare system and trying their best with what they have.
Yet I must express, the pump start up process was haphazardly piecemealed together and poorly communicated, particularly when obtaining initial supplies and making appointments. If not for the navigational persistence garnered by my professional and educational background in healthcare, I’d probably still be at Square One without a pump. I made dozens of calls between Tandem, suppliers, and the Endo clinic, babysitting, “Okay. XYZ is done. What’s the next step?” And many times no one seemed to really know. This bureaucratic disorganization delayed the actual pump start date for weeks.
Many of us have thirty or ninety days’ worth of supplies worked out with insurers and suppliers. We are being asked upfront to spend hundreds of dollars on large orders of infusion sets which may not end up being best for our individual case, for example. Or then the Endo clinic prescribed many boxes of infusion sets but not enough cartridges. The general oversight has been lacking. If not for kindhearted members of the DOC and friends already using Control IQ, I would have been even more lost as I sorted out initial tips and tricks for an ideal pumping experience.
Endo clinics and major diabetes industry names and so on do not have to like me or consult directly with me, per se. But that said, the wisdom of the lived experience is so valuable. (If you believe in real patient advocacy, reimburse such expertise accordingly, by the way). I would be happy to be hired as part of a focus group on formulating a more comprehensive, linear implementation training guide to help clinics, pump companies, and diabetes patients, alike, in safely and successfully getting situated on a new pump. (If your company is interested, feel free to leave contact information in the comments on this page and I will email you back). And again, if not me, please consult with other patient advocates. I am sharing oodles of feedback here because I want people with diabetes to have the best quality of life and health that we can, but a good company will not just take such ideas and run away; this work involves deep, meaningful engagement between all parties.
Cartridge fills / site changes
No matter how many years I’ve been away from pumping, I still grimace on site change days- not so much in terms of acute pain from the needles involved, rather due to time, inconvenience, and complexity. I’m not the first to note that Tandem’s process is tedious; my user guide is Post-It-Note-tabbed to pertinent instructive chapters, which I read at every site change. I’m using “site change” interchangeably with “cartridge change” here, but the latter part is actually the burdensome aspect.
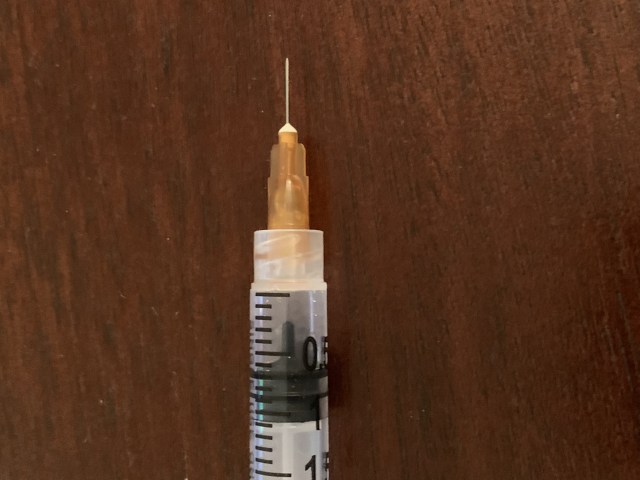
While Tandem’s “inject air into the insulin vial, remove air from cartridge” routine does seem to make a difference in terms of maintaining insulin efficacy within the pump, the cumbersome tools and learning curve to get there could use improvement. The miniscule white cartridge hole where one must insert a ginormous needle to spray hundreds of units of insulin is daunting when first using this pump. What if I accidentally stab my own thumb?!, I can’t help but think each time. Assumedly there are biomedical designs here to keep the insulin clean and secure via the small cartridge hole, but this is an area to seek change. Additionally, many official training videos skip over the actual filling the cartridge with the needle part, but this aspect is so important if we are to avoid air populating the cartridge inadvertently.

Supply Adequacy
The inherently poor design of our American “healthcare system,” by nature, is responsible for this critique. Third party suppliers, diabetes companies, and even healthcare providers’ prescriptions nowadays mainly opt to allot the exact amount of diabetes supplies, with no wiggle room for the inevitable rainy day mishaps. When in doubt, call customer service, they proclaim! Prompting those of us in the trenches to wonder, “Have you ever waited on hold listening to the seventeenth string symphony orchestra practice squad on speakerphone while working fulltime to pay these bills?” Yeah, we didn’t think so.
Companies would save time, and I’d even argue, some money when all comes out in the wash, if they provided even a few spare infusion sets or Dexcom sensors over the course of one year, rather than perpetuating negative experiences when life happens and we need more. Surviving with not one extra centimeter by which to breathe is fundamentally unjust to the customers with health conditions padding these companies’ pockets. Put your customer service energy elsewhere, do the right thing, and eliminate this problem by conceding at least once per order that something may go wrong, but you’re going to own that as a dependable company and provide a back-up option.
Emotional Support
We hear about the transition for Service Members coming home after combat tours and experiencing a tough readjustment to the civilian world. Their guard has been on high alert for months, and now we expect them to just jump back into mowing the lawn, holding down an office job, or socializing at a party, as if the traumas they endured and witnessed never happened?
Although this pump has rocked my world already, there has been an emotional element which I am still similarly processing. On shots, I got accustomed to trying so hard each day and not really witnessing the fruits of that labor very often. The long-term outlook was so grim that I couldn’t even visit there in my mind. Time would eventually just stop, probably.
So I found myself sobbing when a provider recently asked me to go there, to try to imagine a different, better course with the help of this pump. I need more time to heal fully, to reacquaint myself to the light of a calmer world. Such a good thing still hurts because of the tender scar tissue.
Healthcare clinics should at least have this concept on their radar, particularly when training patients who have never pumped before or are returning from sabbatical. These fancy new pumps are jaw-droppingly good at what they do, and that isn’t a bad thing. But the shock and awe mean something, too, and we should strive to optimally support people with diabetes in these next chapters.
Disclosures and disclaimers:
I own Dexcom stock, although this truthfully has no effect on my ultimate aim of improving quality of life for all people with diabetes. No matter what, my feedback will always be candid.
I wrote this blog on my own volition, and although I hope the diabetes industry will listen, these views and ideas are solely my own.
Use diabetes medical devices at your own risk and based on guidance from your medical providers.
This blog is not exhaustive and surely there is more food for thought to come.


I have all kinds of great things to say about the pump and one bad thing. The one bad thing is I want to see inside that damn cartridge. I want to know what is going on inside? Air bubbles, I can deal with that. how much insulin is left? I am not concerned if I can see it. Do I need to change my site early, later, or right on time, give me the chance to make that decision by YES – LET ME LOOK INSIDE. For almost 20 years Medtronic trusted me to look inside and guess what? I DID !!! A lot.
LikeLike
Rick, I love this. So true. I hope Tandem takes note. This is a great idea.
LikeLike