This week will be my final class before graduating with my Master’s degree at the end of December. The saying about a weight being lifted is true. As I handed in my final paper last week and my classmates hoorayed, happy to see one of their own crossing the finish line, I instantly felt relief.
Unless you live under a #doc Twitter rock, you know that I was on an emotional rollercoaster last week. I second-guessed whether I would get my final paper done in time. Mostly, though, that doubt was due to the anxiety of moving forward in life, of leaving behind the structure, love, and discipline that grad school has blessed me with over the past two years.
As much as I have complained about homework on the weekends, truth be told, I will miss the academic environment very much. There is a definable purpose there, a working towards something greater than oneself, a joy of learning amongst peers and professors who are just as passionate about healthcare and making the world a better place.
Grad school becomes a part of one’s identity, and I am scared out of my mind to not cling to that role soon. My go-to introduction spiel at cocktail parties has been, “I’m Ally. I work fulltime at _____ and I go to grad school at night at _____ and have I mentioned how freakin’ busy I am all the darn time?!!” As fulfilling as these different components of my life are, it is now time to put what I have learned to good use and to explore new opportunities- after taking a much-needed vacation.
My identity as a graduate student may be shifting, but I do not necessarily have to be lost. Perhaps I have already been found, and that is what is so scary- those moments of truth where you reconcile who you are, with who you have been, with who you want to be.
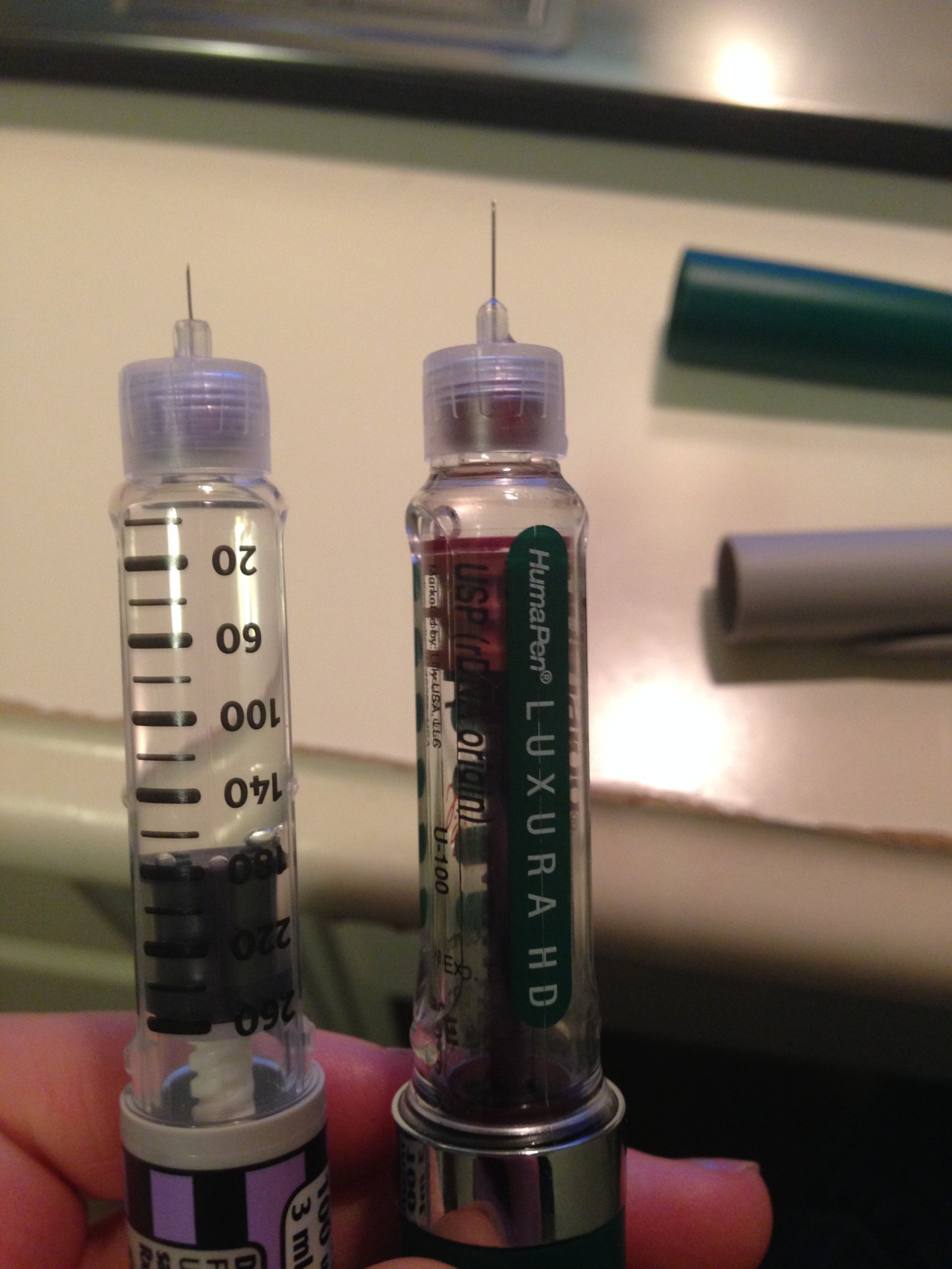
Complicating such notions is the fact that today marks my one year shot-o-versary, or the anniversary of returning to a multiple daily injections regimen after a decade of insulin pumping. I have beaten a dead horse over this, but in case you are new to Very Light, No Sugar: Insulin pumps are great. Sadly, I experienced product defects with mine and watched my health slowly slip away as a result. The pros of using injections for me, personally, outweighed the cons, so here I am. Do what works for you.
My current apathy about the shots milestone surprises me. In many ways I expected to be just as proud about the shots as I am about my impending Master’s. But I’m just… not. Shots are my new normal. Some day that may change (diabetes cure, please!), but for now, this is what I am working with.
And to be honest, I think that apathy is a good thing. It means that I have made peace with some of the previous bitterness, that I have chosen to chalk up the pump company’s ignoring of my email pleas as being due to an overloaded pump rep.’s inbox, even though I know in my heart that was never the case.
I now experience the freedom of insulin getting into my body every time I inject, and those #JerkFaces also known as ketones do not hang around much anymore. I have proven to myself that I am stronger than I ever believed, and that it is good that we have many options in our diabetes management tool boxes.
Every day, I have access to life-sustaining medication, something I will never take for granted again. Others are not as fortunate, and I am attuned to their suffering because my faulty insulin pump taught me what it feels like to lack insulin. It is a brutal, desperate torment. Only insulin can fix it. And while I feel blessed to have escaped my insulin-delivery mishaps, I will always remember and pledge to help those who do not have access to insulin.
I recall emailing my doctors a week into our shots trial and implying, “Hey, I tried. Time to call it quits and return to the pump?” And I remember my dismay at their gentle urging to stick it out one more week, one more month.
Today- one more year- I am happy that I listened. The difficult days are still here. But the good days are back, too. Any day not spent battling ketones on the couch is a day that I must be thankful for, and I am. I just need to work on expressing that more often.
So here it goes:
I am thankful to have enjoyed the opportunity of receiving a graduate-level education. During the days of my insulin pump saga, when the ketones were syrupy-thick in my blood and the couch was my home, grad school was the bright light that I could focus on. I read and read and read and repeatedly told myself that one day I would feel better and have my degree.
Today, I am happy to be here to see that internal mantra come to fruition. Thank you to everyone who has rooted for me along the way. My gratitude is best expressed by leaving you with the prayer said on my long drive to Boston before difficult medical appointments:
“In every circumstance and in all things
I have learned the secret of being well fed
and of going hungry,
of living in abundance and of being in need.
I can do all things in Him who strengthens me.
Still, it was kind of you to share in my distress.”
-Phillipians 4:12-14